9/26/2021
Shiraz Kowsar Hospital, a Center of Excellence for DBS Surgery in Southern Iran
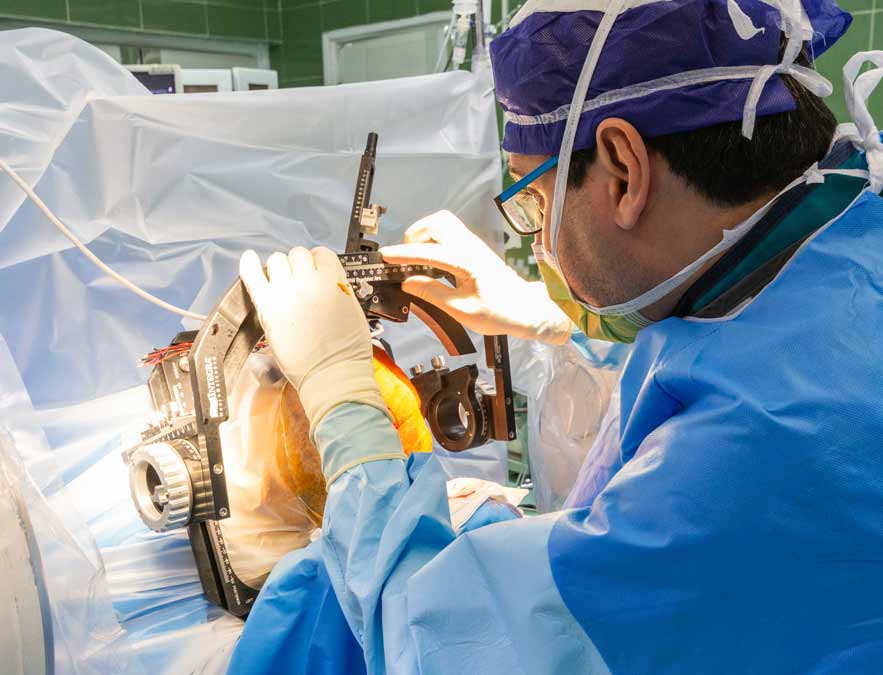
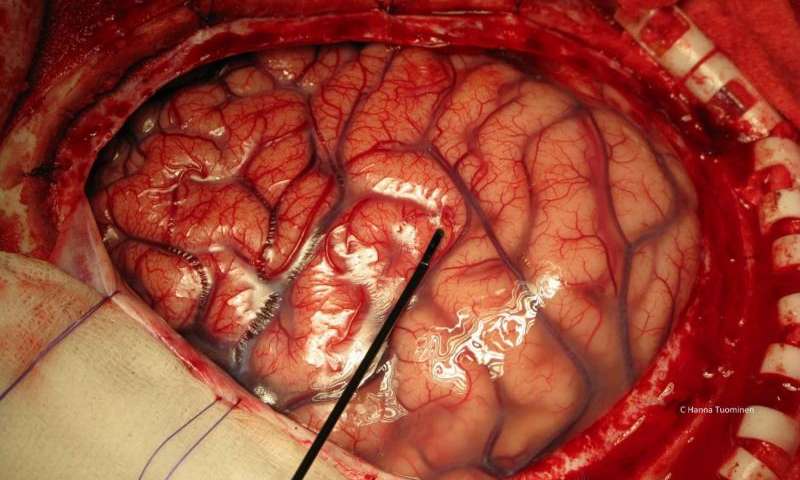
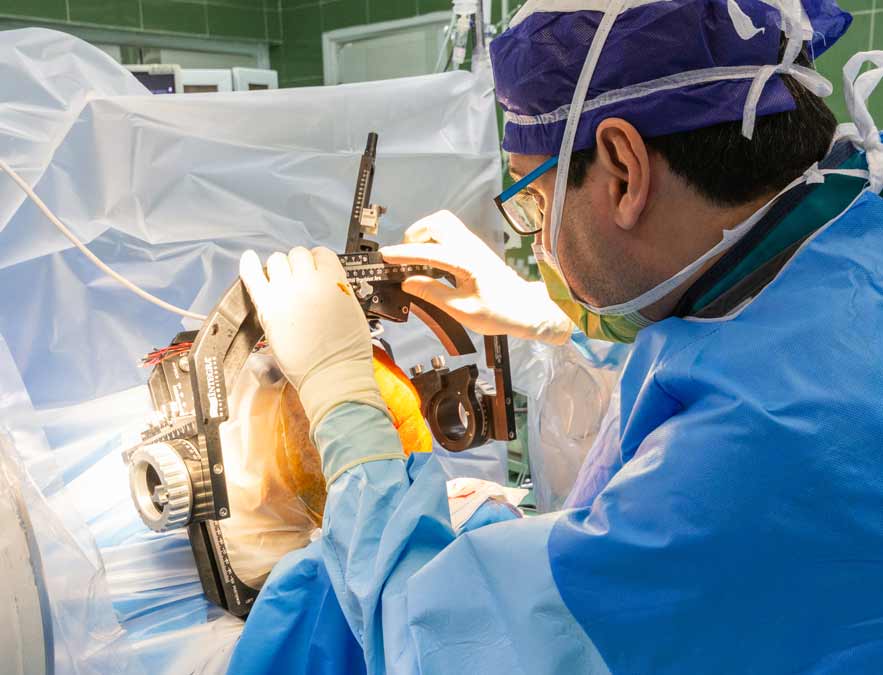
.Shiraz Kowsar Hospital, is currently considered as the main referral center for DBS surgery in Southern Iran
All patients with advanced movement disorders from all over the country are invited to attend our superspecialized clinics to screen for the DBS surgery. Additionally, patients with Obssessive Compulsive Disorder (OCD) and major depression may be considered for Neuromodulation surgeries.




0 Comment
Express your opinion